Outstanding Discovery: AI Is Transforming The Face Of Organ Transplant
AI is Changing the Face of Organ Transplant
Reading Time: 4 minutes
Our Slow Progress in Keeping Organs Viable
One major challenge for the transplant process has always been that organs are so fragile. Keeping them viable outside the body for an extended time period is a near-impossible task, and information gleaned from research shows that their short lifespans differ. While blood can be kept refrigerated for up to six weeks, organs have historically been another story altogether: up until recently, a heart or lung needed to be transplanted within six hours, while a pancreas or liver were only viable for 12 hours. The kidney, exhibiting one of the longest shelf lives, could remain viable for up to 30 hours. Sadly, because of their fragility, some precious donated organs ultimately ended in the waste bin.

Source: Sdecoret/Depositphotos.com
There is an ever-increasing number of people in need of organ transplants. Every 9 minutes, someone is added to the national transplant organ waiting list with an average of 95 successful daily organ transplants taking place in the US. In 2013, 26,517 successful organ transplants were conducted in the United States while over 120,000 patients were stuck on the waiting list. The short window unfortunately did not give physicians much time to identify the proper recipient.
Every 9 minutes, someone is added to the national organ waiting list with an average of 95 successful organ transplants taking place in the US daily.
-US Department of Health and Human Services
Let’s examine the liver: in search of solutions to this age-long conundrum, researchers over the years uncovered several preservation methods. For instance, flushing the organ with a cold solution at time of harvest and then keeping it safe via static storage on ice reduced the rate of metabolic activities and therefore, extended storage up to 18 hours (from the original 12). Later on, another group of scientists figured out that combining supercooling with subzero storage at -4°C with hypothermic and sub-normothermic machine perfusion extended the shelf life to about 27 hours, a fantastic achievement.
Artificial Intelligence to the Rescue?
While these innovations have certainly helped, obstacles remain. It is extremely difficult to repair a damaged liver, and quite a large percentage of them go to waste since they were not healthy enough to be transplanted into the patients in need.
It seems this challenge will soon be met; AI is set to change the face of organ transplant as we know it.
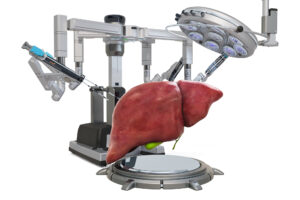
Source: Alexmlx/Depositphotos.com
A group of researchers from the University Hospital Zurich, ETH Zurich, Wyss Zurich, and the University of Zurich has successfully developed an AI-based machine that can repair injured human livers. Their innovation can keep these organs alive outside the human body for up to ONE WEEK, thus saving the lives of more who suffer from cancer and severe liver diseases. The results reveal that six out of ten perfused poor-quality human livers, initially declined for transplantation, recovered full function within a week of perfusion on the machine.
AI-based machine developed by researchers from the University Hospital Zurich and the University of Zurich can preserve injured Human liver for one week.
-Eshmuminov et al. (2020).
The machine was created in line with the Liver4life project from Wyss Zurich, and its intended purpose was to develop a novel therapeutic strategy for liver regeneration including the following:
1) surgical resection of a small healthy piece of the liver from the patient;
2) growth of this piece outside of the body in a perfusion machine until a sufficient size is reached; and
3) re-transplantation of the regenerated liver to the original patient while removing the remaining diseased part.
Their machine was developed in a stepwise fashion using pig livers. The ex vivo parameters and phase reperfusion in vivo were studied to demonstrate the viability of the pig livers perfused for one week without the need for an additional perfusate exchange or blood products. The results were subsequently replicated on ten injured human livers, which were initially rejected for transplantation by all European Centers. Those now-healthy organs demonstrated synthesis of coagulation factors and the production of bile while also maintaining intact liver structure and cellular energy (ATP).
The researchers report that the perfusion machine integrates multiple core physiological functions such as automated hematocrit control, oxygenation, waste product removal, and the management of glucose levels.
The team of researchers, which consisted of biologists, surgeons, and engineers, utilized an algorithm that automatically adjusted the dialysate flow, thus controlling the concentration of hematocrit (red blood cells) with continuous measurements. There was also an automated administration of glucagon and insulin that maintained physiological blood glucose levels, kept at 3.5-6.5mmol-1. Additionally, the machine initiated a continuous movement of the liver that mimicked diaphragm oscillations. All of this was fully automated, which eliminated the need for the constant personnel presence and thus addressed possible physician burnout.
Source: Belchonock/Depositphotos.com
Reaction
While speaking about the project, Prof. Pieere-Allain Clavien, Chairman of the Department of Surgery and Transplantation at the University Hospital Zurich stated: “The success of this unique perfusion system — developed over a four-year period by a group of surgeons, biologists, and engineers — paves the way for many new applications in transplantation and cancer medicine, helping patients with no liver grafts available.”
The machine’s ability to increase the shelf life of livers from just 12 hours to over six days is nothing short of revolutionary. Its utility is not limited to this, however, as it can also repair injury, clean fat deposits, and even regenerate partial livers.
Final words
The reperfusion machine will likely be integral to the future of organ storage and transplant. Although the present research is focused on the liver, there is a great possibility that the project will extend to include other organs. AI is making giant strides and rapidly evolving not just transplantation, but all areas of medicine. Thoughts? Questions? Reach us in the comments below and don’t forget to share this with a friend!










Helena Knight
I pay a visit day-to-day some blogs and sites to read articles, but this website provides quality based
posts.